
Contributions
Abstract: PB2161
Type: Publication Only
Background
Multiple myeloma (MM) is a relatively usual hemato-oncological disease the incidence of which has been increasing. Despite a significant progress in drug development, autologous transplantation (Tx) of peripheral hematopoietic stem cells remains the fundamental pillar of the treatment. The standard administration consists in a dose of melphalan 200 mg/m2, and this regimen is preferably used with younger patients due to the toxicity risk of the preparation regimen. The dose of melphalan can be reduced to 100-180 mg/m2 in older patients depending on the overall patient's condition.
Aims
The objective of our work was to compare the length of hospitalization, event. infection and GIT complications and also the influence on PFS and OS in a group divided by age.
Methods
Retrospective analysis in 179 patients with MM transplanted consecutively in the Department of Hematology and Oncology, University Hospital in Pilsen, between 2013 - 2017. The data evaluation was performed after the first Tx. In all patients, melphalan was only administered as a part of conditioning.
Results
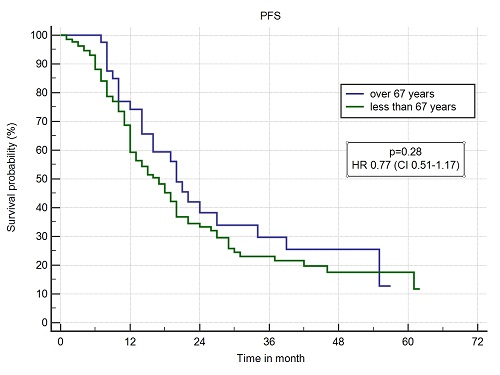
The group of 179 patients was divided by age. In the group of patients > 67 years of age, there were a total of 47 patients with median age 70 (67-75), while the group of patients < 67 years of age at the time of Tx (B) was represented by 133 patients with median age 59 (41-66). Besides age, there was no statistical difference between the basic parameters. In group A, the average dose of melphalan was 154mg/m2, in group B, it was 188mg/m2. The total hospitalization time showed median of 15 days (14-28) in group A and 16 days (13-63) in group B. The engraftment was the same in both groups. Gastrointestinal toxicity was completely comparable - in both groups, the median showed grade I (0-IV), in group A, there was no more serious complication than grade III, in group B there was grade III+IV just in 2%. Infective complications in group A were relatively rare, the median was grade 0 (0-II) with no occurrence of more serious infective complications, in group B, just 1% of very serious infections (gr. III+IV), median of grade I (0-IV). Our analysis did not even show any apparent influence of the lower dose of melphalan on PFS or OS. Median PFS in group A was 20 months and 15 months in group B (p= 0.28, HR 0.77, CI 0.51-1.17). Median OS in group A was not reached and in group B, it was 40 months (p= 0.23, HR 0.66, CI 0.36-1.22).
Conclusion
Autologous transplantation is an integral part of the treatment in patients having the diagnosis of multiple myeloma. So far, it has been standardly used in younger patients, however, our data show that even older patients may be transplant eligible and that it is possible to get the same results as in younger patients including PFS and OS while the toxicity risk remains the same.
Take message home: Autologous Tx with a reduced dose in patients up to 70 years of age is more convenient than regimens based on 'new drugs'.
Session topic: 14. Myeloma and other monoclonal gammopathies - Clinical
Keyword(s): Autologous hematopoietic stem cell transplantation, Melphalan, Multiple Myeloma
Abstract: PB2161
Type: Publication Only
Background
Multiple myeloma (MM) is a relatively usual hemato-oncological disease the incidence of which has been increasing. Despite a significant progress in drug development, autologous transplantation (Tx) of peripheral hematopoietic stem cells remains the fundamental pillar of the treatment. The standard administration consists in a dose of melphalan 200 mg/m2, and this regimen is preferably used with younger patients due to the toxicity risk of the preparation regimen. The dose of melphalan can be reduced to 100-180 mg/m2 in older patients depending on the overall patient's condition.
Aims
The objective of our work was to compare the length of hospitalization, event. infection and GIT complications and also the influence on PFS and OS in a group divided by age.
Methods
Retrospective analysis in 179 patients with MM transplanted consecutively in the Department of Hematology and Oncology, University Hospital in Pilsen, between 2013 - 2017. The data evaluation was performed after the first Tx. In all patients, melphalan was only administered as a part of conditioning.
Results
The group of 179 patients was divided by age. In the group of patients > 67 years of age, there were a total of 47 patients with median age 70 (67-75), while the group of patients < 67 years of age at the time of Tx (B) was represented by 133 patients with median age 59 (41-66). Besides age, there was no statistical difference between the basic parameters. In group A, the average dose of melphalan was 154mg/m2, in group B, it was 188mg/m2. The total hospitalization time showed median of 15 days (14-28) in group A and 16 days (13-63) in group B. The engraftment was the same in both groups. Gastrointestinal toxicity was completely comparable - in both groups, the median showed grade I (0-IV), in group A, there was no more serious complication than grade III, in group B there was grade III+IV just in 2%. Infective complications in group A were relatively rare, the median was grade 0 (0-II) with no occurrence of more serious infective complications, in group B, just 1% of very serious infections (gr. III+IV), median of grade I (0-IV). Our analysis did not even show any apparent influence of the lower dose of melphalan on PFS or OS. Median PFS in group A was 20 months and 15 months in group B (p= 0.28, HR 0.77, CI 0.51-1.17). Median OS in group A was not reached and in group B, it was 40 months (p= 0.23, HR 0.66, CI 0.36-1.22).

Conclusion
Autologous transplantation is an integral part of the treatment in patients having the diagnosis of multiple myeloma. So far, it has been standardly used in younger patients, however, our data show that even older patients may be transplant eligible and that it is possible to get the same results as in younger patients including PFS and OS while the toxicity risk remains the same.
Take message home: Autologous Tx with a reduced dose in patients up to 70 years of age is more convenient than regimens based on 'new drugs'.
Session topic: 14. Myeloma and other monoclonal gammopathies - Clinical
Keyword(s): Autologous hematopoietic stem cell transplantation, Melphalan, Multiple Myeloma


