
Contributions
Abstract: PB1743
Type: Publication Only
Session title: Quality of life, palliative care, ethics and health economics
Background
Higher-risk MDS pts and caregivers face many challenges in the course of disease management. Pts with advanced cancer and their caregivers can experience physical, emotional, social, financial, and functional issues. Research on the burden of caring for advanced cancer pts suggests that there is insufficient support for caregivers, likely due to the lack of knowledge about their needs and burdens. The overall experience of caregivers for MDS pts has not been evaluated to date.
Aims
Identify key challenges for caregivers of higher-risk MDS pts in the (1) caregiver role before, during, and after diagnosis; and along the disease journey; (2) Impact on the caregiver’s life and well-being; consequently their areas of need for support; (3) Impact of decisions made, including treatments.
Methods
The OBB was the qualitative research methodology used. OBB enables data collection via a web-based platform. This innovative type of online focus group can generate more meaningful and impactful insights compared to traditional focus groups. A mix of moderator-led Q&A and participant discussion provides the caregiver insights as online dialogue. OBB is advantageous when participants are located in various geographic locations, time zones, and availabilities. Additionally, such a virtual platform meant the research was not disrupted despite being conducted during the COVID-19 pandemic. Inclusion criteria: (1) caregiver of adult pt with high- or very high-risk MDS as diagnosed per IPSS-R category or high-risk MDS as per IPSS, or intermediate-risk pts on hypomethylating agents, and (2) Proficiency in written English. Exclusion criteria: (1) Caregiver of pt with lower-risk MDS; (2) caregiver of pt in a clinical trial; and (3) Paid caregiver.
Results
16 caregivers participated: 5 from the US, 6 from the UK, and 5 from Canada. A content analysis identified 7 key themes where caregiver burden was significant (Table).
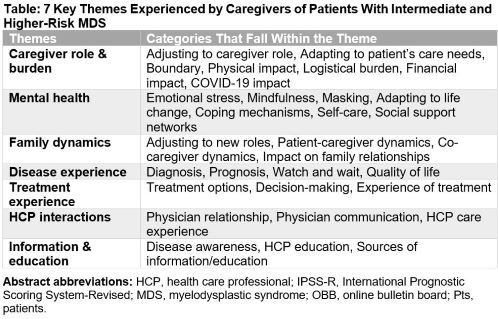
Conclusion
The findings highlight a significant impact and burden on caregivers of pts with higher-risk MDS, which varies depending on the stage of the disease, the choice (or lack of choice) of treatments, and the personal situation of the caregiver. For example, although the caregiver role for more recently diagnosed pts is perceived as minimal effort, their role increases significantly if a stem cell transplant occurs, and/or if there are changes in the pt’s health status (eg, infection, medication change, managing side effects). Emotional stress is pervasive, especially at diagnosis and prognosis stage, and when told to “watch and wait.” This is amplified when HCPs are perceived to lack knowledge/expertise about MDS, resulting in additional burden to pts and caregivers as they seek more appropriate care. There is a strong need for mental health support for both pt and caregiver. The extent required depends on the personal situation and dynamics of the pt and caregiver. Additional stress factors include the uncertainty of employment and financial burden; the time burden when balancing other commitments; and the impact on their own health, particularly if they have their own health issues to manage. Most caregivers can manage the physical and functional aspects of care; however, many state that the bigger unmet need for both pt and caregiver is emotional support, which has not typically been part of the standard of care provided to MDS pts. There is thus an opportunity for healthcare systems to provide better support in these areas of emotional burden.
Keyword(s): Caregiver, MDS, Qualitative, Quality of life
Abstract: PB1743
Type: Publication Only
Session title: Quality of life, palliative care, ethics and health economics
Background
Higher-risk MDS pts and caregivers face many challenges in the course of disease management. Pts with advanced cancer and their caregivers can experience physical, emotional, social, financial, and functional issues. Research on the burden of caring for advanced cancer pts suggests that there is insufficient support for caregivers, likely due to the lack of knowledge about their needs and burdens. The overall experience of caregivers for MDS pts has not been evaluated to date.
Aims
Identify key challenges for caregivers of higher-risk MDS pts in the (1) caregiver role before, during, and after diagnosis; and along the disease journey; (2) Impact on the caregiver’s life and well-being; consequently their areas of need for support; (3) Impact of decisions made, including treatments.
Methods
The OBB was the qualitative research methodology used. OBB enables data collection via a web-based platform. This innovative type of online focus group can generate more meaningful and impactful insights compared to traditional focus groups. A mix of moderator-led Q&A and participant discussion provides the caregiver insights as online dialogue. OBB is advantageous when participants are located in various geographic locations, time zones, and availabilities. Additionally, such a virtual platform meant the research was not disrupted despite being conducted during the COVID-19 pandemic. Inclusion criteria: (1) caregiver of adult pt with high- or very high-risk MDS as diagnosed per IPSS-R category or high-risk MDS as per IPSS, or intermediate-risk pts on hypomethylating agents, and (2) Proficiency in written English. Exclusion criteria: (1) Caregiver of pt with lower-risk MDS; (2) caregiver of pt in a clinical trial; and (3) Paid caregiver.
Results
16 caregivers participated: 5 from the US, 6 from the UK, and 5 from Canada. A content analysis identified 7 key themes where caregiver burden was significant (Table).

Conclusion
The findings highlight a significant impact and burden on caregivers of pts with higher-risk MDS, which varies depending on the stage of the disease, the choice (or lack of choice) of treatments, and the personal situation of the caregiver. For example, although the caregiver role for more recently diagnosed pts is perceived as minimal effort, their role increases significantly if a stem cell transplant occurs, and/or if there are changes in the pt’s health status (eg, infection, medication change, managing side effects). Emotional stress is pervasive, especially at diagnosis and prognosis stage, and when told to “watch and wait.” This is amplified when HCPs are perceived to lack knowledge/expertise about MDS, resulting in additional burden to pts and caregivers as they seek more appropriate care. There is a strong need for mental health support for both pt and caregiver. The extent required depends on the personal situation and dynamics of the pt and caregiver. Additional stress factors include the uncertainty of employment and financial burden; the time burden when balancing other commitments; and the impact on their own health, particularly if they have their own health issues to manage. Most caregivers can manage the physical and functional aspects of care; however, many state that the bigger unmet need for both pt and caregiver is emotional support, which has not typically been part of the standard of care provided to MDS pts. There is thus an opportunity for healthcare systems to provide better support in these areas of emotional burden.
Keyword(s): Caregiver, MDS, Qualitative, Quality of life


